As 2016 came to a close last December, I was feeling great. After a busy and tiring first semester, life at my job as a charter school administrator was hectic but starting to stabilize. My two-year-old son was becoming more fun by the day as his language skills developed and his personality started to shine through. And best of all, I was almost halfway through a healthy and {so far} uneventful second pregnancy with a baby due at the end of May. As New Year’s Eve approached, I was excited for 2017 and all the joy and excitement I was sure it would bring. The only thing hanging over my head as we celebrated Christmas with my in-laws and New Year’s with my family was a doctor’s appointment I had scheduled for the day after I returned home. Eight months prior, back in April, I had noticed a fairly large lump in my left breast. At the time, a doctor diagnosed it as fibrocysitc breasts, a common and benign breast condition, but due to growth and changes in the lump during my pregnancy, my OB wanted to take another look.
So on January 4th, the day after I returned from an idyllic two weeks celebrating the holidays with family and friends, I drove to the hospital for my appointment. I was confident that my age, as well as the fact that a previous ultrasound had shown only benign breast tissue, meant that this appointment would be quick and easy as well. I even had my husband stay home with our two year old even though he had to work that day because I was sure the appointment would be quick and I could come home and relieve him shortly. But unlike back in April, when the technician placed the ultrasound wand on my breast, I saw it – a large black spot, clearly a mass of some sort, within the lump. She took note of it and measured it. And then, as she moved the wand, there was another one a few inches away.
After the ultrasound, the radiologist came in and told me that the two masses could be a lot of things, but that she wanted to get a mammogram that day and a biopsy soon just to be sure. At this point I was concerned but still optimistic that it would be nothing. I knew that pregnancy could cause breast changes and assumed that was what we were seeing. After all, I had read the statistics that 80% of breast lumps turn out to be benign, and I was only 30 years old. I exercised, ate healthy, and had breastfed my son for a year. Cancer didn’t happen to people like me; I was sure of it. The technician led me to another room where I had the uncomfortable experience of my first mammogram with my belly draped in lead vests to protect the baby. In hindsight, when the scan finished the way the technician causally asked “and there’s no one here with you today, right?” should have been a clue that something was wrong. That she knew I was about to get the kind of news that you want to hear with a loved one holding your hand and not while sitting in a cold hospital room alone. But it didn’t register. She led me back to a small room where I thought I was going to schedule my biopsy, and as I rested my hand on my belly and felt my baby kick, the radiologist entered the room and told me I had cancer.
Technically, breast cancer can’t be officially diagnosed without a biopsy, but the mammogram showed calcifications in my breast that essentially always mean breast cancer. The radiologist told me that we would have to wait for the biopsy results for an official diagnosis, but she also said that she was so sure it was cancer that if the pathology report came back negative, she would question whether or not the biopsy was done correctly. To be honest, the obviousness of my cancer was also one of its silver linings – while many women describe the wait between their initial mammogram, their biopsy, and the results of the biopsy as agonizing, I didn’t experience that at all. I went from unsuspecting to diagnosed immediately. Additionally, because the imaging made the diagnosis all but certain, the staff at the breast center scrambled to make things official. They scheduled my biopsy for the next morning, even coming in early to make it happen. Two days after my first appointment, my OB/GYN called to let me know that at the age of 30, while 20 weeks pregnant, I had been diagnosed with Invasive Ductal Carcinoma – commonly known as breast cancer.
The next few weeks were filled with doctor’s appointments – I met with a breast surgeon, my OB/GYN, a high-risk OB/GYN, a medical oncologist, and a radiation oncologist – as well as the depressing task of telling family and close friends about my diagnosis. My mom, a ten-year breast cancer survivor, flew out immediately and attended many of my doctor’s appointments with me. I am incredibly fortunate to live near a top-rated cancer center with an incredible oncologist who has studied pregnancy-associated breast cancer for a decade and has treated many, many pregnant patients. Within two weeks of my diagnosis, we met and she determined that I would start chemotherapy immediately. My team of doctors decided I would receive four cycles of IV chemo, one every three weeks. Then, I would recover from chemo for a month and have a unilateral mastectomy at 35 weeks pregnant. After that I would have another month or so before my due date, and once my baby was born, my oncologist would give me a month to breastfeed on my remaining breast before starting a second chemo drug. Following chemo I would do five to six weeks of daily radiation treatment and then start on hormone therapy for a decade.
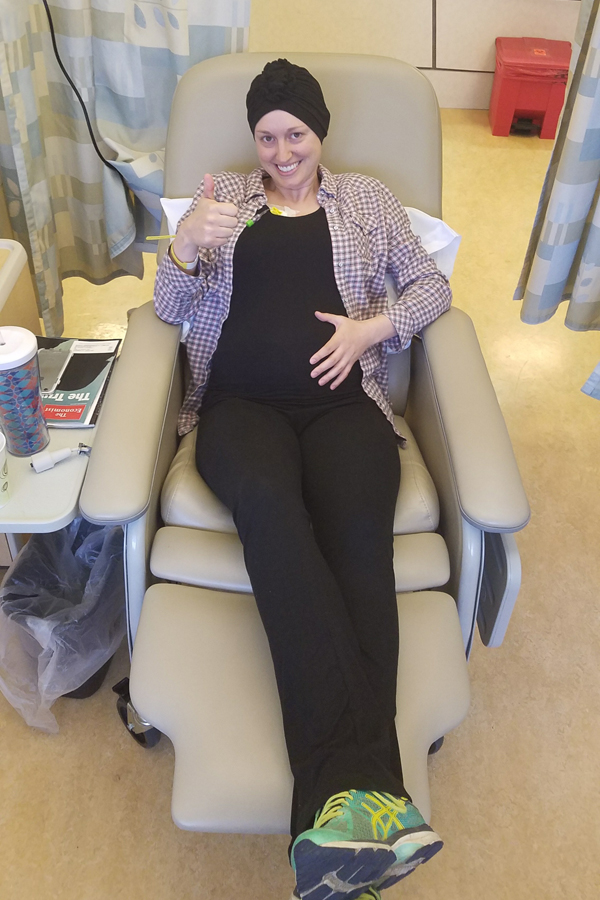
On January 19th, I had a port placed under my skin to deliver chemotherapy directly into my veins {avoiding needing an IV each time}, and on January 24th, I sat in the chemo chair for the first time and watched as a cocktail of drugs dripped into me over a four-hour period. For reasons no doctor has been able to explain to me, pregnant women tend to handle chemotherapy much better than other patients. I took a week off of work each chemo week in preparation for intense side effects, but I found that I felt mostly normal throughout the 12-week process. I was able to work, play with my toddler, and set up a nursery in preparation for my baby’s arrival. In fact, I made a point of setting aside time each week to devote to my unborn baby. In so many ways, my pregnancy was completely usurped by my cancer diagnosis. I hated wearing a wig, so I rarely did in public. But I also hated stares and looks of pity from strangers, so I avoided small talk, even when it was about my bump, for fear that it would turn to questions about my bald head. Unlike my first pregnancy, I wasn’t able to imagine meeting my baby, snuggling, and bonding, without also imagining giving up breastfeeding a month in to go back to the chemo chair. But in many ways I was able to compartmentalize and spend time thinking just about the baby, washing onesies, and decorating the nursery.

On April 20th, I was taken into an operating room where I underwent a unilateral mastectomy. A labor and delivery nurse sat next to me during the entire surgery monitoring the baby’s heartrate. When I woke up from the surgery, the first thing I remember was groggily asking if I was still pregnant, and the nurse kindly reassuring me that the baby had done just fine. Although I was happy to be done with treatment until after childbirth, mastectomy recovery was incredibly difficult. I couldn’t drive myself anywhere for two weeks, which meant relying on my husband or kind family members who flew out to help. I was forbidden from lifting my toddler for six weeks. And for three weeks, I had two tubes coming out from under my skin that drained into pouches I had to empty multiple times a day after recording how much fluid was collecting in them. The surgical site was painful, and although I was prescribed narcotics to manage the pain, I felt incredibly guilty every time I had to take pain medication. During my first pregnancy, I didn’t even take Tylenol. Additionally, the emotional toll of losing a breast – of having a body part so wrapped up in womanhood, sexuality, and childrearing sliced off and discarded – was not something for which I was prepared. But slowly I recovered. I felt better, stopped taking pain medication, and was able to get out and walk. And my hair started to grow back, to the point where I stopped looking like a cancer patient and could comfortably go out without a hat. My friends held a perfect “sprinkle” for our baby, and we put finishing touches in the nursery. On May 20th, I woke up to my water breaking, and six hours later our little chemo baby, Graham David, entered the world perfectly healthy with more hair on his head than me.
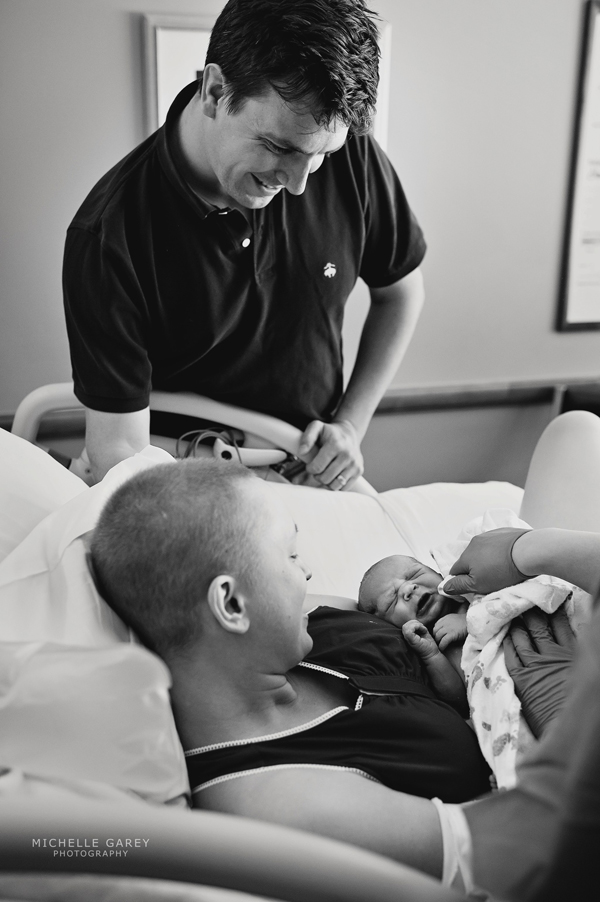
After a few weeks of blissful newborn snuggles and bonding, I headed back to the hospital for more chemo. Although I was incredibly thankful that baby Graham didn’t have to endure additional treatments with me, being back at it was hard. The second chemo drug was easier on the body, but side effects were significantly harder to take while also caring for a newborn. After a three month break from chemo, my hair had finally grown out to a cute, pixie cut length. Although I expected losing it would be easier the second time, I still cried as watched it fall out in the shower. And I had to give up breastfeeding to resume chemo. While I know that formula is a healthy, nutritious alternative to breastmilk, ending our breastfeeding relationship because of chemo – because cancer had taken one more thing away from me – was devastating.
I finished my four rounds of chemo eight weeks after I started, on August 22nd. Three weeks after that, I started daily radiation treatment. Currently, five days a week I leave my baby and toddler with a babysitter and drive to the hospital where I lie on a table while a machine whirs around me, radiating my left side. I am currently three weeks into a six week course of treatment. Once radiation is over, I’ll start hormone treatment which involves a monthly shot to shut down my ovaries and put me into menopause as well as a pill I’ll take daily for ten years. Depending on how my skin handles radiation, I’ll have reconstructive surgery in the next few months as well.
As I approach the end of the “active” portion of my treatment, I’ve started to reflect on the last 10 months. In many ways, I know how lucky I am to have access to great doctors, wonderful friends, and family who have supported me every step of the way, and two happy, healthy little boys. Some days I feel at peace with my diagnosis and confident that soon this will all be behind me. Other days I lie awake at night wondering if I’ll get to see my children’s weddings, their high school graduations, or even Graham’s first day of kindergarten. Because there is no cure for breast cancer, the fear that it will come back will likely be hanging over my head for the rest of my life.

For a long time after my diagnosis I couldn’t look at pictures from Christmas and New Year’s of 2016 because seeing myself right before everything changed was too painful. That person smiling at the camera, hand on her belly, had no doubt she would live a long and happy life. She was looking forward to the rest of a healthy, easy pregnancy and years of fun, excitement, and time with her growing family. But I am also grateful for the perspective I’ve gained. I recently read a blog post by another young cancer survivor where she talked about how before cancer, she had a fifty year plan – that is, she expected she had fifty or so years of life left in which to do all the things she hoped to do. After cancer, she has held onto that fifty year plan, but now she has a five year plan as well. My fifty year plan looks the same as it did in December of 2016. There are so many places I want to visit, things I want to do, and goals I want to achieve throughout the next fifty years. But cancer has made me recognize that no one is guaranteed tomorrow, and life is too short to spend on things that don’t matter. So I have a five year plan now, too. It involves making incredible memories with my kids whenever possible, spending time with my husband and my family, and focusing on the good.
There is so much we can’t control in life, no matter how hard we try, but if I have learned anything over the past 10 months it is to take time to look for the good, the happy, the wonderful, even when it is hard to see. My oncologist demonstrated this during our first appointment. When she entered the exam room two weeks after my diagnosis, my whole world felt like it had just been destroyed. All I could think about was the cancer growing in me. My husband and I sat together on the small chairs in her office, holding hands, looking absolutely terrified I’m sure. I expected her to immediately launch into a conversation about cancer stages, treatment, and survival statistics. Instead, she looked at our fearful, desperate faces, and then down at my bulging baby belly. She looked back at me and smiled. “Congratulations,” she said.
 About Valerie L.
About Valerie L.
Valerie Luckenbill lives in the mountains outside of Denver, Colorado with her husband, two sons, and two dogs.















HI Valerie,
Thank you for sharing your experience. Do you mind me asking what type of breast cancer you have? was there lymph note involve. And what type of chemo did they give you during pregnancy? I am recently diagnosed with Stage II breast cancer and I had a unilateral mastectomy four weeks ago. I am currently 24 weeks pregnant with my 2nd. The doctors wanted me to start AC treatment during pregnancy maybe in a few weeks. But I was not given the green light to breastfeed. So I wanted in your situation how are you able to get that month of bonding time. As mine sounds like wanted me to start the 2nd type of chemo as soon as I am ready.
Thank you for sharing.
Vivian
Hi Vivian,
I am so sorry, I just saw this! I was diagnosed with Invasive Ductal Carcinoma, grade 3. ER+/PR+/HER2-. At my mastectomy (which was after 4 rounds of AC) I had 4 positive nodes. There was evidence of extranodal extension so honestly, it could have been more than four nodes positive originally and the chemo reduced a few. Because I had my mastectomy after AC, I had a long time between chemo and childbirth which is why breastfeeding was ok and my doctor was also comfortable giving me a few weeks between childbirth and taxol but I have met other women in the same situation whose doctors are not comfortable so it may be a case by case basis.
I’m not sure where you are in your treatment or if any decisions have been made but please feel free to email me. I am part of a Facebook group for women diagnosed with cancer while pregnant and it has been very helpful to speak to other women about their experiences. My email address is [email protected]. I would also recommend reaching out to Dr. Cardonick at the Hope for Two Network (http://www.hopefortwo.org/dr-elyce-cardonick-obgyn-maternal-fetal-medicine-specialist/) as she has significant experience helping pregnant patients navigate treatment decisions, including breastfeeding safety.
Again, I am so sorry I didn’t see this. I hope you are doing ok and please feel free to reach out if you think it would be helpful!